Chapter 246-225 WAC
Last Update: 6/1/17RADIATION PROTECTION—X-RAYS IN THE HEALING ARTS
WAC Sections
| HTMLPDF | 246-225-001 | Purpose and scope. |
| HTMLPDF | 246-225-010 | Definitions. |
| HTMLPDF | 246-225-020 | General requirements—Administrative controls. |
| HTMLPDF | 246-225-030 | General requirements—Plan review. |
| HTMLPDF | 246-225-040 | General requirements for diagnostic X-ray systems. |
| HTMLPDF | 246-225-050 | Fluoroscopic X-ray systems. |
| HTMLPDF | 246-225-060 | Radiographic systems other than fluoroscopic, dental intraoral, or veterinary systems—Beam limitation. |
| HTMLPDF | 246-225-070 | Radiographic systems other than fluoroscopic, dental intraoral, or veterinary systems—Radiation exposure control devices. |
| HTMLPDF | 246-225-080 | Radiographic systems other than fluoroscopic, dental intraoral, or veterinary systems—Source-to-skin or receptor distance. |
| HTMLPDF | 246-225-090 | Radiographic systems other than fluoroscopic and dental intraoral—Exposure reproducibility. |
| HTMLPDF | 246-225-100 | Radiographic systems—Standby radiation from capacitor energy storage equipment. |
| HTMLPDF | 246-225-120 | Therapeutic X-ray installations less than 1 MeV. |
| HTMLPDF | 246-225-130 | X-ray and electron therapy systems with energies of one MeV and above. |
| HTMLPDF | 246-225-140 | Veterinary medicine radiographic installations. |
| HTMLPDF | 246-225-150 | X-ray film developing requirements. |
| HTMLPDF | 246-225-160 | Mammography. |
| HTMLPDF | 246-225-99920 | Appendix II—Determination of competency. |
| HTMLPDF | 246-225-99930 | Appendix III—Information to be submitted by persons proposing to conduct healing arts screening using ionizing radiation. |
DISPOSITION OF SECTIONS FORMERLY CODIFIED IN THIS TITLE
| 246-225-110 | Intraoral dental radiographic systems. [Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-110, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-110, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 83-19-050 (Order 2026), § 402-28-080, filed 9/16/83. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-080, filed 12/8/80; Order 1084, § 402-28-080, filed 1/14/76; Order 1, § 402-28-080, filed 1/8/69; Rules (part), filed 10/26/66.] Repealed by WSR 08-14-074, filed 6/26/08, effective 7/27/08. Statutory Authority: RCW 70.98.050 and 70.98.080. |
| 246-225-99910 | Appendix I—Good practices. [Statutory Authority: RCW 70.98.050. WSR 94-01-073, § 246-225-99910, filed 12/9/93, effective 1/9/94. Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-99910, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-99910, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 83-19-050 (Order 2026), § 402-28-99001, filed 9/16/83; Order 1084, Appendix D (codified as WAC 402-28-99001), filed 1/14/76.] Repealed by WSR 97-20-101, filed 9/29/97, effective 10/30/97. Statutory Authority: RCW 43.70.040. |
PDF246-225-001
Purpose and scope.
This chapter establishes requirements, for which a registrant is responsible, for use of X-ray equipment by or under the supervision of an individual authorized by and licensed in accordance with state statutes to engage in the healing arts. The provisions of this chapter are in addition to, and not in substitution for, other applicable provisions of these regulations.
[Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-001, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-010, filed 12/8/80; Order 1084, § 402-28-010, filed 1/14/76; Order 1, § 402-28-101 (codified as WAC 402-28-010), filed 1/8/69; Rules (part), filed 10/26/66.]
PDF246-225-010
Definitions.
As used in this chapter, the following definitions apply:
(1) "Accessible surface" means the external surface of the enclosure or housing provided by the manufacturer.
(2) "Accidental radiation exposure incident" means an exposure to a patient, an operator, or a member of the public that was unintentional.
(3) "Added filter" means the filter added to the inherent filtration.
(4) "Aluminum equivalent" means the thickness of aluminum (type 1100 alloy) affording the same attenuation, under specified conditions, as the material in question. (The nominal chemical composition of type 1100 aluminum alloy is 99.00 percent minimum aluminum, 0.12 percent copper.)
(5) "Assembler" means any person engaged in the business of assembling, replacing, or installing one or more components into an X-ray system or subsystem. An assembler may be the practitioner, his/her employee, an outside contractor, or an employee of an outside firm.
(6) "Attenuation block" means a block or stack, having dimensions 20 cm by 20 cm by 3.8 cm, of type 1100 aluminum alloy or other aluminum alloys having equivalent attenuation.
(7) "Automatic exposure control" means a device which automatically controls one or more technique factors in order to obtain at a preselected location(s) a required quantity of radiation (see also "phototimer").
(8) "Barrier" (see "protective barrier").
(9) "Beam axis" means a line from the source through the centers of the X-ray fields.
(10) "Beam-limiting device" means a device which provides a means to restrict the dimensions of the X-ray field.
(11) "Beam monitoring system" means a system designed to detect and measure the radiation present in the useful beam.
(12) "C-arm X-ray system" means an X-ray system in which the image receptor and X-ray tube housing assembly are connected by a common mechanical support system in order to maintain a desired spatial relationship. This system is designed to allow a change in the projection of the beam through the patient without a change in the position of the patient.
(13) "Cephalometric device" means a device intended for the radiographic visualization and measurement of the dimensions of the human head.
(14) "Certified components" means components of X-ray systems which have been certified by the manufacturer as meeting the requirements of the federal performance standard for X-ray equipment.
(15) "Certified system" means any X-ray system which has one or more certified component(s).
(16) "Changeable filters" means any filter, exclusive of inherent filtration, which can be removed from the useful beam through any electronic, mechanical or physical process.
(17) "Coefficient of variation (C)" means the ratio of the standard deviation to the mean value of a population of observations. It is estimated using the following equation:
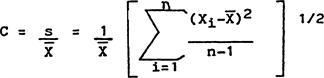 |
where | |
s = Estimated standard deviation of the population. | |
X = Mean value of observations in sample. | |
X(i ) = ith observation sampled. | |
n = Number of observations in sample. | |
(18) "Contact therapy system" means an X-ray system wherein the X-ray tube port is put in contact with or within 5 centimeters of, the surface being treated.
(19) "Control panel" means that part of the X-ray control upon which are mounted the switches, knobs, pushbuttons, and other hardware necessary for manually setting the technique factors.
(20) "Cooling curve" means the graphical relationship between heat units stored and cooling time.
(21) "Date of transfer." See installation date.
(22) "Dead-man switch" means a switch so constructed that a circuit closing contact can be maintained only by continuous pressure on the switch by the operator.
(23) "Department" means the department of health which has been designated as the state radiation control agency.
(24) "Detector" (see "radiation detector").
(25) "Diagnostic source assembly" means the tube housing assembly with a beam-limiting device attached.
(26) "Diagnostic X-ray system" means an X-ray system designed for irradiation of any part of the human or animal body for the purpose of recording or visualization for diagnostic purposes.
(27) "Direct scattered radiation" means that scattered radiation which has been deviated in direction only by materials irradiated by the useful beam (see also "scattered radiation").
(28) "Electronic product defect" means an error in design, manufacture, or performance of an X-ray system such that unintentional radiation exposure to a patient, an operator, or a member of the public has occurred.
(29) "Entrance exposure rate" means the exposure measured free-in-air per unit time where the useful beam enters the patient.
(30) "Equipment" (see "X-ray equipment").
(31)*"Exposure" means the quotient of dQ divided by dm where dQ is the absolute value of the total charge of the ions of one sign produced in air when all the electrons (negatrons and positrons) liberated by photons in a volume element of air having mass dm are completely stopped in air. (The special unit of exposure is the roentgen.)
Note: | *When the word, exposure, is used in this part to mean one or more irradiations of a person for a healing arts purpose, or in a more general sense, it will not be underlined. |
(32) "Field emission equipment" means equipment which uses an X-ray tube in which electron emission from the cathode is due solely to the action of an electric field.
(33) "Filter" means material placed in the useful beam to absorb preferentially selected radiations.
(34) "Fluoroscopic imaging assembly" means a component which comprises a reception system in which X-ray photons produce a fluoroscopic image. It includes equipment housings, electrical interlocks if any, the primary protective barrier, and structural material providing linkage between the image receptor and the diagnostic source assembly.
(35) "Focal spot" means the area on the anode of the X-ray tube bombarded by the electrons accelerated from the cathode, and from which the useful beam originates.
(36) "Full beam detector" means a radiation detector of such size that the total cross section of the maximum size useful beam is intercepted.
(37) "General purpose radiographic X-ray system" means any radiographic X-ray system which, by design, is not limited to radiographic examination of specific anatomical regions.
(38) "Gonad shield" means a protective barrier for the testes or ovaries.
(39) "Half-value layer (HVL)" means the thickness of specified material which attenuates the beam of radiation to an extent such that the exposure rate is reduced to one-half of its original value. In this definition the contribution of all scattered radiation, other than any which might be present initially in the beam concerned, is deemed to be excluded.
(40) "Healing arts screening" means the testing of an asymptomatic population using X-ray machines for the detection or evaluation of health indications when such tests are not specifically and individually ordered by a licensed practitioner of the healing arts legally authorized to prescribe such X-ray tests for the purpose of diagnosis or treatment.
(41) "Heat unit" means a unit of energy equal to the product of the peak kilovoltage, miliamperes, and seconds, i.e., kVp x mA x second.
(42) "Image intensifier" means a device consisting of an image intensifier tube installed in its housing which instantaneously converts an X-ray pattern into a light image of higher energy density.
(43) "Image receptor" means any device, such as a fluorescent screen or radiographic film, which transforms incident X-ray photons either into a visible image or into another form which can be made into a visible image by further transformations.
(44) "Image receptor support" means that part of a mammographic system designed to support the image receptor in a plane perpendicular to the X-ray beam during mammography.
(45) "Inherent filtration" means the filtration of the useful beam provided by the permanently installed components of the tube housing assembly.
(46) "Installation date" means the earliest date that a machine, accessory, or component is able to be used by a registrant or transferee but no later than the date of the first human exposure made using the machine, accessory, or component that has been installed.
(47) "Interlock" means a device arranged or connected such that the occurrence of an event or condition is required before a second event or condition can occur or continue to occur.
(48) "Irradiation" means the exposure of matter to ionizing radiation.
(49) "Kilovolts peak (kVp)" (see "peak tube potential").
(50) "kV" means kilovolts.
(51) "kWs" means kilowatt second which is equal to the product of peak kilovolts, amperes, and seconds or 10-3 X kV X mA X sec.
(52) "Lead equivalent" means the thickness of lead affording the same attenuation, under specified conditions, as the material in question.
(53) "Leakage radiation" means radiation emanating from the diagnostic or therapeutic source assembly except for:
(a) The useful beam and
(b) Radiation produced when the exposure switch or timer is not activated.
(54) "Leakage technique factors" means the technique factors associated with the tube housing assembly which are used in measuring leakage radiation. They are defined as follows:
(a) For capacitor energy storage equipment, the maximum rated peak tube potential and the maximum rated number of exposures in an hour for operation at the maximum rated peak tube potential with the quantity of charge per exposure being 10 milliampere seconds, or the minimum obtainable from the unit, whichever is larger.
(b) For field emission equipment rated for pulsed operation, the maximum rated peak tube potential and the maximum rated number of X-ray pulses in an hour for operation at the maximum rated peak tube potential.
(c) For all other equipment, the maximum rated peak tube potential and the maximum rated continuous tube current for the maximum rated peak tube potential.
(55) "Light field" means that area of the intersection of the light beam from the beam-limiting device and one of the set of planes parallel to and including the plane of the image receptor, whose perimeter is the locus of points at which the illumination is one-fourth of the maximum in the intersection.
(56) "Line-voltage regulation" means the difference between the no-load and the load line potentials expressed as a percent of the load line potential; that is,
Percent | |||
line-voltage = 100 (Vn-V1)/V1 | |||
regulation | |||
where: | |||
V(n) = No-load line potential | |||
V(1) = Load line potential | |||
(57) "mA" means tube current in milliamperes.
(58) "mAs" means milliampere second or the product of the tube current in milliamperes and the time of exposure in seconds.
(59) "Maximum line current" means the root mean squared current in the supply line of an X-ray machine operating at its maximum rating.
(60) "Mobile equipment" (see "X-ray equipment").
(61) "Modified installation" means a room, building, office, or facility in which structural parameters which affect radiation safety are being changed; these parameters include such things as reconstruction or moving of walls, replacement of the X-ray machine with one of higher kVp or mA, a change in the direction of the beam, replacement of the control panel so that operator protection is adversely affected, a change in occupancy of adjacent areas, workload changes, etc.
(62) "New installation" means a room, building, office, or facility newly built, or in which previously there has been no radiation machine.
(63) "Peak tube potential" means the maximum value of the potential difference across the X-ray tube during an exposure.
(64) "Phantom" means a volume of material similar to tissue with respect to attenuation and scattering of X-ray photons. This requires that the atomic number (Z) and the density of the material be similar to those of tissue.
(65) "Phototimer" - means a device which controls radiation exposure to the image receptor by detecting the total amount of radiation reaching the device. The radiation monitoring device(s) is part of an electronic circuit which controls the time the tube is activated (see also "automatic exposure control").
(66) "Portable equipment" (see "X-ray equipment").
(67) "Position indicating device (PID)" means a device, on dental X-ray equipment which indicate the beam position and establishes a definite source-surface (skin) distance. The device may or may not incorporate or serve as a beam-limiting device.
(68) "Positive beam limitation" means the automatic or semi-automatic adjustment of an X-ray beam to the selected image receptor size, whereby exposures cannot be made without such adjustment.
(69) "Primary protective barrier" (see "protective barrier").
(70) "Protected area" means a shielded area in which attenuation of x-radiation is sufficient to meet the exposure limits of WAC 246-221-010 and the principles of WAC 246-220-007 and "ALARA" for individuals in that area.
(71) "Protective apron" means an apron made of radiation absorbing materials, used to reduce radiation exposure.
(72) "Protective barrier" means a barrier of radiation absorbing material(s) used to reduce radiation exposure.
(a) "Primary protective barrier" means the material, excluding filters, placed in the useful beam, to protect anyone other than the patient from radiation exposure.
(b) "Secondary protective barrier" means a barrier sufficient to attenuate the stray radiation to the required degree.
(73) "Protective glove" means a glove made of radiation absorbing materials used to reduce radiation exposure.
(74) "Quality assurance" is a program designed to produce high quality radiographs at minimal cost and minimal patient exposure.
(75) "Quality control" is the routine measurement of the performance of the diagnostic X-ray imaging system, from X-ray beam output to the viewing of radiographs, and the continual adjustment of that performance to an optimal and consistent level.
(76) "Radiation detector" means a device which in the presence of radiation provides by either direct or indirect means, a signal or other information suitable for use in measuring one or more quantities of incident radiation.
(77) "Radiation safety" means efforts directed at occupational exposure reduction, patient exposure reduction, image quality improvement, diagnostic imaging system quality assurance, radiation measurements, dose evaluations, compliance with state and federal regulations, and related issues.
(78) "Radiation therapy simulation system" means a fluoroscopic or radiographic X-ray system intended for localizing the volume to be exposed during radiation therapy and confirming the position and size of the therapeutic irradiation field.
(79) "Radiograph" means an image receptor on which the image is created directly or indirectly by an X-ray pattern and results in a permanent record.
(80) "Radiographic imaging system" means any system whereby a permanent or temporary image is recorded on an image receptor by the action of ionizing radiation.
(81) "Rating" means the operating limits of an X-ray system or subsystem as specified by the component manufacturer.
(82) "Recording" means producing a permanent form of an image resulting from X-ray photons (e.g., film, video tape).
(83) "Response time" means the time required for an instrument system to reach 90 percent of its final reading when the radiation-sensitive volume of the instrument system is exposed to a step change in radiation flux from zero sufficient to provide a steady state midscale reading.
(84) "Scattered radiation" means radiation that, during passage through matter, has been deviated in direction (see also "direct scattered radiation").
(85) "Secondary protective barrier" (see "protective barrier").
(86) "Shutter" means a device attached to the tube housing assembly which can totally intercept the entire cross sectional area of the useful beam and which has a lead equivalency at least that of the tube housing assembly.
(87) "SID" (see "source-image receptor distance").
(88) "Source" means the focal spot of the X-ray tube.
(89) "Source-image receptor distance (SID)" means the distance from the source to the center of the input surface of the image receptor.
(90) "Source-to-skin-distance (SSD)" means the distance between the source and the skin entrance plane of the patient.
(91) "Special purpose X-ray equipment" means that which is designed for radiographic examination of one specific area of the body.
(92) "Spot check" means an abbreviated calibration procedure which is performed to assure that a previous calibration continues to be valid.
(93) "Spot film device" means a device intended to transport and/or position a radiographic image receptor between the X-ray source and fluoroscopic image receptor, including a device intended to hold a cassette over the input end of an image intensifier for the purpose of making a radiograph.
(94) "Spot film" means a radiograph which is made during a fluoroscopic examination to record permanently conditions which exist during that fluoroscopic procedure.
(95) "Stationary equipment" (see "X-ray equipment").
(96) "Stray radiation" means the sum of leakage and scattered radiation.
(97) "Technique factors" means the conditions of operation. They are specified as follows:
(a) For capacitor energy storage equipment, peak tube potential in kV and quantity of charge in mAs.
(b) For field emission equipment rated for pulsed operation, peak tube potential in kV and number of X-ray pulses.
(c) For all other equipment, peak tube potential in kV and:
(i) Either tube current in mA and exposure time in seconds,
(ii) Or the product of tube current and exposure time in mAs.
(98) "Transmission detector" means a radiation detector through which the useful beam or part of the useful beam passes.
(99) "Treatment volume" means the region, in the patient, to which a specified dose is to be delivered.
(100) "Tube" means an X-ray tube, unless otherwise specified.
(101) "Tube housing assembly" means the tube housing with tube installed. It includes high-voltage and/or filament transformers and other appropriate elements when they are contained within the tube housing.
(102) "Tube rating chart" means the set of curves which specify the rated limits of operation of the tube in terms of the technique factors.
(103) "Useful beam" means the radiation which passes through the tube housing port and the aperture of the beam-limiting device when the exposure switch or timer is activated.
(104) "Variable-aperture beam-limiting device" means a beam-limiting device which has capacity for stepless adjustment of the X-ray field size.
(105) "Visible area" means that portion of the input surface of the image receptor over which incident X-ray photons produce a visible image.
(106) "Wedge filter" means an added filter with changing radio-opacities used to achieve more uniform optical densities on the image receptor when a body part of varying absorption characteristics is radiographed.
(107) "X-ray control" means a device which controls input power to the X-ray high-voltage generator and/or the X-ray tube. It includes equipment which controls the technique factors of an X-ray exposure.
(108) "X-ray equipment" means an X-ray system, subsystem, or component thereof. Types of X-ray equipment are as follows:
(a) 'Mobile' means X-ray equipment mounted on a permanent base with wheels and/or casters for moving while completely assembled.
(b) 'Portable' means X-ray equipment designed to be hand-carried.
(c) 'Stationary' means X-ray equipment which is installed in a fixed location.
(109) "X-ray field" means that area of the intersection of the useful beam and any one of the set of planes parallel to and including the plane of the image receptor, whose perimeter is the locus of points at which the exposure rate is one-fourth of the maximum in the intersection.
(110) "X-ray high-voltage generator" means a device which transforms electrical energy from the potential supplied by the X-ray control to the tube operating potential. The device may also include means for transforming alternating current to direct current, filament transformers for the X-ray tube(s), high-voltage switches, electrical protective devices, and other appropriate elements.
(111) "X-ray system" means an assemblage of components for the controlled production of x-rays. It includes minimally an X-ray high-voltage generator, an X-ray control, a tube housing assembly, a beam-limiting device, and the necessary supporting structures. Additional components which function with the system are considered integral parts of the system.
(112) "X-ray subsystem" means any combination of two or more components of an X-ray system for which there are requirements specified in this part.
(113) "X-ray tube" means any electron tube which is designed to be used primarily for the production of X-rays.
[Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-010, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-010, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 83-19-050 (Order 2026), § 402-28-020, filed 9/16/83. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-020, filed 12/8/80; Order 1084, § 402-28-020, filed 1/14/76; Order 1, § 402-28-020, filed 1/8/69; Rules (part), filed 10/26/66.]
PDF246-225-020
General requirements—Administrative controls.
(1) No person shall make, sell, lease, transfer, lend, or install X-ray equipment or the accessories used in connection with such equipment unless such accessories and equipment, when properly placed in operation and properly used, shall meet the requirements of this chapter.
(2) The registrant in control of the X-ray machines shall be responsible for directing the operation of the X-ray machines. The registrant or registrant's agent shall assure the following provisions are met in the operation of the X-ray machine or machines:
(a) The registrant shall not operate an X-ray machine for diagnostic or therapeutic purposes when the X-ray machine:
(i) Does not meet the provisions of this chapter; or
(ii) Is malfunctioning and threatens the health or safety of the patient, operator, or general public.
(b) X-ray machine operator requirements.
(i) Individuals operating the X-ray equipment shall be adequately instructed in safe operating procedures and shall be able to demonstrate competence, upon request from the department, in the correct use of the equipment. Required areas of competence are listed in Appendix II. The department may determine compliance with subsection (2)(b) of this section by observation, interview, or testing;
(ii) A medical X-ray machine operator shall be licensed, certified or registered by the department as either:
(A) A health care practitioner, licensed under Title 18 RCW; or
(B) A diagnostic or therapeutic radiologic technologist certified in accordance with chapter 18.84 RCW; or
(C) An X-ray technician registered in accordance with chapter 18.84 RCW.
(c) At each X-ray system's control panel, a chart shall be provided which specifies for the examinations performed by that system the following information:
(i) Patient's anatomical size versus technique factors utilized;
(ii) Source to image receptor distance used;
(iii) Type and placement of patient shielding used, for example, gonad, thyroid, lap apron;
(iv) If applicable, settings for automatic exposure devices; and
(v) Type and size of film or screen-film combination to be used.
(d) When required by the department, a registrant shall create and provide to operators of the X-ray system, radiation safety procedures which address patient and occupationally exposed personnel safety. These procedures shall define restrictions of the operating technique required for safe operation of the particular X-ray system;
(e) Except for patients who cannot be moved out of the room and the patient being examined, only the staff and ancillary personnel required for the medical procedure or training shall be present in the room during the radiographic exposure. Other than the patient being examined:
(i) All individuals shall be positioned such that no part of the body including the extremities not protected by 0.5 mm lead equivalent will be struck by the useful beam;
(ii) The X-ray operator, other staff and ancillary personnel shall be protected from the direct scatter radiation by protective aprons or whole body protective barriers of not less than 0.25 mm lead equivalent;
(iii) Patients who cannot be removed from the room shall be:
(A) Protected from the direct scatter radiation by whole body protective barriers of not less than 0.25 mm lead equivalent; or
(B) Positioned so the nearest portion of the body is at least 2 meters from both the tube head and the nearest edge of the image receptor.
(iv) The department may require additional protective devices when a portion of the body of staff or ancillary personnel is potentially subjected to stray radiation which may result in that individual receiving one quarter of the maximum permissible dose defined under WAC 246-221-010.
(f) Gonad shielding of not less than 0.5 mm lead equivalent shall be used for patients of reproductive age during radiographic procedures in which the gonads are in the direct (useful) beam, except for cases when gonad shielding may interfere with the diagnostic procedure;
(g) Persons shall not be exposed to the useful beam except for healing arts purposes. Only a licensed practitioner of the healing arts shall authorize an exposure to the useful beam. This requirement prohibits deliberate exposure for the following purposes:
(i) Exposure of an individual for training, demonstration, or other purposes unless there are also healing arts requirements and proper prescription is provided;
(ii) Except for mammography performed by registered facilities on self-referred patients, the exposure of an individual for the purpose of healing arts screening without prior written approval of the state health officer; and
(iii) Exposure of an individual for the sole purpose of satisfying a third party's prerequisite for reimbursement under any health care plan, except for exposure required under medicare provisions.
(h) When a patient or film must be provided with auxiliary support during a radiation exposure:
(i) Mechanical holding devices shall be used when the technique permits. The safety rules, when required under subdivision (d) of this subsection, shall list individual projections where holding devices cannot be utilized;
(ii) Written safety procedures, when required under subdivision (d) of this subsection, shall indicate the requirements for selecting a human holder and the procedure the holder shall follow;
(iii) The human holder shall be protected as required under subdivision (e)(i) of this subsection;
(iv) No person shall be used routinely to hold film or patients;
(v) When the patient must hold the film, the portion of the body other than the area of clinical interest struck by the useful beam shall be protected by not less than 0.5 mm lead equivalent material;
(vi) Holding the film or the patient shall be permitted only in very unusual and rare situations.
(i) Personnel dosimetry. All persons associated with the operation of an X-ray system are subject to both the occupational exposure limits and the requirements for the determination of the doses stated under WAC 246-221-020. In addition, when protective clothing or devices are worn on portions of the body and a dosimeter is required, at least one such dosimeter shall be utilized as follows:
(i) When an apron is worn, the monitoring device shall be worn at the collar outside of the apron; and
(ii) The dose to the whole body based on the maximum dose attributed to the most critical organ shall be recorded on the reports required under WAC 246-221-230. If more than one device is used or a record is made of the data, each dose shall be identified with the area where the device was worn on the body.
(iii) Personnel monitoring of an operator shall be required where:
(A) Exposure switch cords are utilized that allow the operator to stand in an unprotected area during exposures; and
(B) Measurements by the department show ten percent of the exposure limits as specified under WAC 246-221-010 may be exceeded.
(iv) All persons involved in the operation of a fluoroscope and working within the fluoroscopy room during its operation shall wear a personnel dosimeter required under WAC 246-221-090 and subsection (2)(i)(i) of this section. If extremities are in or near the primary beam, extremity dosimeters are also required;
(j) Healing arts screening utilizing radiation. Any person proposing to conduct a healing arts screening program, with the exception of a mammography program, shall not initiate such a program without prior approval of the state health officer. When requesting such approval, that person shall submit the information outlined under Appendix III of this part. If information submitted becomes invalid or outdated, the state health officer shall be notified immediately;
(k) When using scatter suppressing grids, the grids shall be:
(i) Clearly labelled with the focal distance for which they are designed to be used; and
(ii) Of the proper focal distance for the source-to-image distances used.
(l) Procedures and auxiliary equipment designed to minimize patient and personnel exposure commensurate with the needed diagnostic information shall be utilized.
(i) Film cassettes without intensifying screens shall not be used for any routine diagnostic radiological imaging.
(ii) Portable or mobile X-ray equipment shall be used only for examinations where it is impractical to transfer the patient(s) to a stationary X-ray installation.
(m) Patient log. A medical X-ray facility (chiropractors, allopathic and osteopathic physicians and hospitals only) shall record for each X-ray diagnosis or treatment the patient's name, type of X-ray procedures performed, and the date. A separate log is not necessary if the required information is retrievable by reference to other records.
[Statutory Authority: RCW 70.98.050. WSR 94-06-017, § 246-225-020, filed 2/22/94, effective 3/25/94. Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-020, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-020, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 87-01-031 (Order 2450), § 402-28-031, filed 12/11/86; WSR 83-19-050 (Order 2026), § 402-28-031, filed 9/16/83. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-031, filed 12/8/80; Order 1084, § 402-28-031, filed 1/14/76. Formerly WAC 402-28-030 (part).]
PDF246-225-030
General requirements—Plan review.
(1) Before construction, the floor plans and equipment arrangement of medical installations (new or modifications of existing installations) utilizing X-rays for diagnostic or therapeutic purposes shall be submitted to:
(a) A qualified expert for determination of shielding requirements using National Council on Radiation Protection and Measurements (NCRP) Report No. 147, available at the NCRP website at https://www.ncrppublications.org, or equivalent; and
(b) The department for subsequent review.
Review shall not imply approval.
(2) The review of such plans shall not preclude the requirement of additional modifications should a subsequent analysis of operating conditions indicate the possibility of an individual receiving a dose in excess of the limits required under WAC 246-221-010, 246-221-050, and 246-221-060.
(3) Diagnostic veterinary, podiatric, and dental facilities shall be exempt from submitting shielding calculations and floor plans.
(4) In order for the department to provide an evaluation, technical advice, and official review of the shielding requirements for a medical radiation installation, a floor plan drawn to scale and the following data are required:
(a) The normal location of the X-ray tube, along with an indication of anode-cathode orientation to the cassette holders;
(b) The limits of the tube travel;
(c) The directions in which the tube is pointed;
(d) Window locations;
(e) The location of the control booth or operator's position;
(f) The exposure switch location;
(g) The position of the viewing window, if any;
(h) The composition and thickness of the walls;
(i) If more than one story, the height floor-to-floor;
(j) If more than one story, the composition and thickness of materials in the ceiling or floor;
(k) The make and model of the X-ray machine;
(l) The maximum kVp and mA;
(m) The types of examinations or treatments (for example, chest, spine, general X-ray, or therapy);
(n) The identification and occupancy of areas adjacent to the X-ray room;
(o) The anticipated X-ray workload expressed in number of patients and exposures per week including:
(i) Technique factors used, or milliampere-seconds or milliampere-minutes per week; and
(ii) Estimates of the percentage of the workload expected to occur for a particular beam direction.
(5) For new and modified installations only, the following are minimum design requirements for medical X-ray machine operator booths. These requirements do not apply to dental, podiatry, and veterinary installations. See subsections (6) and (7) of this section for dental panoramic and cephalometric requirements.
(a) The operator shall be allotted 0.7 sq. meters (7.5 sq. ft.) or more of unobstructed floor space in the X-ray booths.
(i) The 0.7 sq. meters (7.5 sq. ft.) of minimum space specified under subsection (5)(a) of this section shall be a geometric configuration where no dimension is less than 61.0 centimeters (2.0 ft.).
(ii) The allotted space shall exclude an encumbrance by the console, such as an overhang, cables, or other similar encroachment.
(iii) An extension of a straight line drawn between any point on the edge of the booth shielding and the nearest vertical edge of a vertical cassette holder, corner of the examination table, or any part of the tube housing assembly shall not impinge on the unobstructed space.
(iv) The booth walls shall be 2.1 meters (7.0 ft.) or more and shall be permanently fixed to the floor or other structure as may be necessary.
(v) When a door or moveable panel is used as the integral part of the booth structure, it must have a permissive device which will prevent an exposure when the door or panel is not closed.
(b) Switch placement. The operator's switch for the radiographic machine shall be fixed within the booth. The switch shall:
(i) Be at least 102 centimeters (forty inches) inside the protected area; and
(ii) Allow the operator to use the available viewing windows.
(c) Viewing system requirements.
(i) Each booth shall have at least one viewing device which shall:
(A) Be placed so the operator can view the patient during exposure; and
(B) Be placed so the operator can have full view of the entries into the room.
(ii) When the viewing system is a window, the following requirements also apply:
(A) The window shall have a visible area of 930 square centimeters (1.0 square foot) or more; and
(B) The glass shall have the same lead equivalence or more as that required in the booth's wall where the glass is mounted.
(iii) When the viewing system is by mirrors, the mirrors shall be located to accomplish the general requirements under subdivision (i) of this subsection.
(iv) When the viewing system is by electronic means (for example, TV):
(A) The camera shall be located to accomplish the general requirements under subdivision (i) of this subsection; and
(B) There shall be an alternate viewing system as a backup for electronic failure.
(d) New or modified facilities shall maintain a copy of the floor plan and shielding calculations required under subsection (1) of this section.
(6) Dimensions of primary beam shielding shall exceed the largest possible beam size by 30.5 centimeters (one foot) or more in every direction. Cephalometric primary beam shielding shall be deemed adequate if, for a maximum workload of twenty films a week, two-pound lead is installed (for occupied areas).
(7) A viewing device shall be present in dental panoramic and cephalometric X-ray installations, so the requirements of subsection (5)(c) of this section are met.
[Statutory Authority: RCW 70.98.010, 70.98.050, and 70.98.080. WSR 17-12-046, § 246-225-030, filed 6/1/17, effective 7/2/17. Statutory Authority: RCW 70.98.050. WSR 94-01-073, § 246-225-030, filed 12/9/93, effective 1/9/94. Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-030, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-030, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 87-01-031 (Order 2450), § 402-28-032, filed 12/11/86; WSR 83-19-050 (Order 2026), § 402-28-032, filed 9/16/83; Order 1084, § 402-28-032, filed 1/14/76. Formerly WAC 402-28-030 (part).]
PDF246-225-040
General requirements for diagnostic X-ray systems.
In addition to other requirements of this chapter, diagnostic X-ray systems shall meet the following requirements:
(1) Warning label. The control panel containing the main power switch shall bear the warning statement, legible and accessible to view: "warning: This X-ray unit may be dangerous to patient and operator unless safe exposure factors and operating instructions are observed."
(2) Battery charge indicator. On battery-powered generators, visual means shall be provided on the control panel to indicate the battery is in a state of charge adequate for proper operation.
(3) Leakage radiation from the diagnostic source assembly. The leakage radiation from the diagnostic source assembly, measured at a distance of 1 meter in any direction from the source, shall not exceed 2.58 x 10-5 coulombs per kilogram (100 milliroentgens) in one hour when the X-ray tube is operated at its leakage technique factors. Compliance shall be determined by measurements averaged over an area of one hundred square centimeters with no linear dimension greater than twenty centimeters.
(4) Radiation from components other than the diagnostic source assembly. The radiation emitted by a component other than the diagnostic source assembly shall not exceed 5.16 x 10-7 coulombs per kilogram (2 milliroentgens) in one hour at 5 centimeters from an accessible surface of the component when it is operated in an assembled X-ray system under conditions for which it was designed. Compliance shall be determined by measurements averaged over an area of 100 square centimeters with no linear dimension greater than 20 centimeters.
(5) Beam quality.
(a) The half-value layer (HVL) of the useful beam for a given X-ray tube potential shall not be less than the values shown in this section, Table I. If it is necessary to determine such half-value layer at an X-ray tube potential which is not listed in Table I, linear interpolation or extrapolation shall be made.
WAC 246-225-040 TABLE 1
Design operating range (kilovolts peak) | Measured potential (kilovolts peak) | Half-value layer (milli- meters of aluminum equivalent) | Half-value layer (milli- meter of aluminum equivalent for dental units) | |||
Below 51–– | 30 | 0.3 | N/A | |||
40 | 0.4 | N/A | ||||
50 | 0.5 | 1.5 | ||||
51 to 70––– | 51 | 1.2 | 1.5 | |||
60 | 1.3 | 1.5 | ||||
70 | 1.5 | 1.5 | ||||
Above 70–– | 71 | 2.1 | 2.1 | |||
80 | 2.3 | 2.3 | ||||
90 | 2.5 | 2.5 | ||||
100 | 2.7 | 2.7 | ||||
110 | 3.0 | 3.0 | ||||
120 | 3.2 | 3.2 | ||||
130 | 3.5 | 3.5 | ||||
140 | 3.8 | 3.8 | ||||
150 | 4.1 | 4.1 | ||||
(b) For capacitor energy storage equipment, compliance shall be determined with the system fully charged and a setting of at least 10 mAs for each exposure.
(c) The required minimal half-value layer shall include the filtration contributed by materials permanently in position between the focal spot of the tube and the patient. (For example, a table top when the tube is mounted "under the table" and inherent filtration of the tube.)
(d) Filtration control. For X-ray systems with variable kVp and variable filtration for the useful beam, a device shall link the kVp selector with the filters and shall prevent an exposure unless the minimum amount of filtration required by subdivision (a) of this subsection is in the useful beam for the selected kVp.
(6) Multiple tubes. Where two or more radiographic tubes are controlled by one exposure switch, the tube or tubes selected shall be clearly indicated prior to initiation of the exposure. Such indication shall be both on the X-ray control panel and near or on the selected tube housing assembly.
(7) Mechanical support of tube head. The tube housing assembly supports shall be adjusted such that the tube housing assembly remains stable during an exposure unless the tube housing movement during exposure is a designed function of the X-ray system.
(8) Technique indicators.
(a) The technique factors used during an exposure shall be indicated before the exposure begins, except when automatic exposure controls are used, in which case the technique factors set prior to the exposure shall be indicated.
(b) On equipment having fixed technique factors, the requirement, under subdivision (a) of this subsection may be met by permanent markings. Indication of technique factors shall be visible from the operator's position except in the case of spot films made by the fluoroscopist.
(9) Certified units. All diagnostic X-ray systems certified to comply with 21 C.F.R. 1020 shall meet the requirements of that certification.
(10) Linearity. The difference between the ratio of exposure to mAs at one mA or mAs setting and the ratio at another mA or mAs setting shall not exceed 0.10 times the sum of the ratios. This is written as:
X1 - X2 ≤ 0.10 (X1 + X2) |
Where X1 and X2 are the ratios (mR/mAs) for each mA or mAs station.
The test shall be performed at any selections of mA or mAs without regard to focal spot size, provided neither focal spot size is less than 0.45 millimeter.
(11) kVp accuracy. The difference between the indicated and actual kVp of an X-ray machine shall not be greater than ten percent of the indicated kVp, or, alternatively, if available, the accuracy specifications of the control panel manufacturer must be met.
[Statutory Authority: RCW 70.98.050. WSR 94-01-073, § 246-225-040, filed 12/9/93, effective 1/9/94. Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-040, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-040, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 87-01-031 (Order 2450), § 402-28-035, filed 12/11/86; WSR 83-19-050 (Order 2026), § 402-28-035, filed 9/16/83. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-035, filed 12/8/80; Order 1084, § 402-28-035, filed 1/14/76. Formerly WAC 402-28-030 (part).]
PDF246-225-050
Fluoroscopic X-ray systems.
Fluoroscopic X-ray systems shall meet the following requirements:
(1) Limitation of useful beam.
(a) The fluoroscopic tube shall not produce X-rays unless the primary barrier is in position to intercept the entire useful beam at all times.
(b) The entire cross section of the useful beam shall be intercepted by the primary protective barrier of the fluoroscopic image assembly at any source-to-image-distance (SID).
(c) Nonimage-intensified fluoroscopic equipment shall not be used.
(d) For fluoroscopic equipment without a spot film device, neither the length nor the width of the fluoroscopic X-ray field in the plane of the image receptor shall exceed that of the visible area of the image receptor by more than three percent of the SID. The sum of the excess length and the excess width shall be no greater than four percent of the SID. Measurements shall be made at the minimum SID available but at no less than 20 centimeters (8 inches) table top to image receptor distance.
(e) For uncertified fluoroscopic equipment with a spot film device, the fluoroscopic X-ray beam with the shutters wide open (during either fluoroscopy itself or spot films) shall be no larger than the dimensions of the largest spot film size for which the device is designed. Measurements shall be made at the minimum SID available, but at no less than 20 centimeters (8 inches) table top to the film plane distance.
(f) For certified (21 C.F.R. 1020) fluoroscopic equipment with a spot film device, neither the length nor the width of the fluoroscopic X-ray field in the plane of the image receptor shall exceed that of the visible area of the image receptor by more than three percent of the SID. The sum of the excess length and width shall be no greater than four percent of the SID. Measurements shall be made at the minimum SID available, but at no less than 20 centimeters (8 inches) table top to film plane distance.
(g) Fluoroscopic equipment beam limitation:
(i) Means shall be provided to reduce the beam size at the plane of the image receptor to 125 square centimeters or less; and
(ii) The minimum field size at the greatest SID shall be equal to or less than 5 centimeters by 5 centimeters.
(2) Activation of the fluoroscopic tube. X-ray production in the fluoroscopic mode shall be controlled by a deadman switch.
(3) Entrance exposure rate allowable limits.
(a) For equipment with or without automatic brightness control, the exposure rate measured at the point where the center of the useful beam enters the patient shall not exceed 2.58 x 10-3 coulombs per kilogram per minute (ten roentgens per minute), except during film recording of fluoroscopic images or when an optional high level control (HLC) is activated.
(b) For equipment provided with HLC, the equipment shall not be operable at a combination of tube potential and current which will result in an exposure rate in excess of 1.29 x 10-3 coulombs per kilogram per minute (5 roentgens per minute) at the point where the center of the useful beam enters the patient, unless the HLC is activated.
(i) Special means of activation of high level controls, such as additional pressure applied continuously by the operator, shall be required to avoid accidental use.
(ii) A continuous signal audible to the fluoroscopist shall indicate the high level control is employed.
(c) Measuring compliance of entrance exposure rate limits. Compliance with subsection (3) of this section shall be determined as follows:
(i) Movable grids and compression devices shall be removed from the useful beam during the measurement;
(ii) If the source is below the table, exposure rate shall be measured 1 centimeter above the table top or cradle;
(iii) If the source is above the table, the exposure rate shall be measured at 30 centimeters above the table top with the end of the beam-limiting device or spacer positioned as closely as possible to the point of measurement;
(iv) In a C-arm type of fluoroscope, the exposure rate shall be measured 30 centimeters from the input surface of the fluoroscopic imaging assembly, with the source positioned at any available SID, provided the end of the beam-limiting device or spacer is no closer than 30 centimeters from the input surface of fluoroscopic imaging assembly; and
(v) In a lateral-type fluoroscope, the exposure rate shall be measured at a point 15 centimeters from the center line of the X-ray table with the end of the beam-limiting device or spacer positioned as closely as possible to the point of measurement. If the table top is movable, the table top shall be positioned as closely as possible to the lateral X-ray source, with the end of the beam-limiting device or spacer no closer than 15 centimeters to the center line of the X-ray table.
(d) Periodic measurement of entrance exposure rate limits.
(i) Periodic measurements of the exposure rate shall be made. An adequate period for such measurements shall be annually or after maintenance of the system affecting the exposure rate.
(ii) Results of exposure rate measurements shall be available where the fluoroscopist has ready access to the measurements while using that fluoroscope. Results of the measurements shall include:
(A) The maximum possible coulombs per kilogram per minute (R/minute), as well as the technique factors associated with it;
(B) The name of the person performing the measurements;
(C) The last date the measurements were performed; and
(D) The type of device used in making the measurements.
(iii) Conditions of measurement:
(A) The kVp shall be adjusted to that which will produce the maximum entrance exposure rate;
(B) The high level control, if present, shall not be activated;
(C) The X-ray systems that incorporate automatic exposure rate control (automatic brightness control) shall have sufficient material, for example, lead or lead equivalence, placed in the useful beam to produce the maximum output of the X-ray system; and
(D) X-ray systems not incorporating automatic exposure rate control shall utilize whatever combination of kVp, mA, and other selectable parameters that will generate the highest exposure rate of the X-ray system. Materials, for example, an attenuation block, may be placed in the useful beam to protect the imaging system, as long as the material does not affect the measurement of the exposure rate.
(4) Barrier transmitted radiation rate limits.
(a) The exposure rate due to transmission through the primary protective barrier with the attenuation block in the useful beam, combined with radiation from the image intensifier, if provided, shall not exceed 5.16 x 10-7 coulombs per kilogram per hour (2 milliroentgens per hour) for each 2.58 x 10-4 coulombs per kilogram per minute (roentgen per minute) of entrance exposure rate. The barrier transmission measurement shall be made at 10 centimeters from an accessible surface of the fluoroscopic imaging assembly beyond the plane of the image receptor.
(b) Measuring compliance of barrier transmission.
(i) The exposure rate due to transmission through the primary protective barrier combined with radiation from the image intensifier shall be determined by measurements averaged over an area of 100 square centimeters with no linear dimension greater than 20 centimeters.
(ii) If the source is below the table top, the measurement shall be made with the input surface of the fluoroscopic imaging assembly positioned 30 centimeters above the table top.
(iii) If the source is above the table top and the SID is variable, the measurement shall be made with the end of the beam-limiting device or spacer as close to the table top as it can be placed, provided the beam-limiting device or spacer shall not be closer than 30 centimeters.
(iv) Movable grids and compression devices shall be removed from the useful beam during the measurement.
(5) Indication of potential and current. During fluoroscopy and cinefluorography, X-ray tube potential and current shall be continuously indicated.
(6) Source-skin distance (SSD). The source to skin distance shall not be less than:
(a) 38 centimeters on stationary fluoroscopes;
(b) 30 centimeters on mobile fluoroscopes; and
(c) 20 centimeters for image intensified fluoroscopes used for specific surgical application. The user must provide precautionary measures for the use of the fluoroscope due to its short SSD.
(7) Fluoroscopic timer.
(a) Means shall be provided to preset the cumulative on-time of the fluoroscopic tube. The maximum cumulative time of the timing device shall not exceed five minutes without resetting.
(b) A signal audible to the fluoroscopist shall indicate the completion of a preset cumulative on-time. Such signal shall continue to sound while X-rays are produced until the timing device is reset. Alternatively, the timing device may terminate exposures at the end of the preset time.
(c) Total fluoroscopic on-time for each patient shall be recorded, either in patient's chart or in a separate log.
(8) Control of scattered radiation.
(a) Fluoroscopic table designs when combined with normal operating procedures shall be such that no unprotected part of staff or ancillary person's body shall be exposed to unattenuated scattered radiation which originates from under the table. The attenuation required shall be not less than 0.25 mm lead equivalent.
(b) Equipment configuration when combined with procedures shall be such that no portion of staff or ancillary person's body, except the extremities, shall be exposed to the unattenuated scattered radiation emanating from above the table top unless:
(i) The radiation has passed through not less than 0.25 mm lead equivalent material, for example, drapes, Bucky-slot cover-sliding or folding panel, or self-supporting curtains, in addition to lead equivalency provided by the protective apron referred to under WAC 246-225-020 (2)(e); and
(ii) Exceptions to subdivision (b) of this subsection may be made in some special procedures where a sterile field will not permit the use of the normal protective barriers. Where the use of prefitted sterilized covers for the barriers is practical, the department shall not permit such exception.
(9) Radiation therapy simulation systems. Radiation therapy simulation systems shall be exempt from the requirements of subsection (3) of this section. In addition, these systems shall be exempt from:
(a) Subsections (1) and (4) of this section provided such systems are designed and used in such a manner that no individual other than the patient is in the X-ray room when the system is producing X-rays; and
(b) Subsection (7) of this section if such systems are provided with a means of indicating the cumulative time that an individual patient has been exposed to X-rays.
[Statutory Authority: RCW 70.98.050. WSR 94-01-073, § 246-225-050, filed 12/9/93, effective 1/9/94. Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-050, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-050, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 87-01-031 (Order 2450), § 402-28-040, filed 12/11/86; WSR 83-19-050 (Order 2026), § 402-28-040, filed 9/16/83. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-040, filed 12/8/80; Order 1084, § 402-28-040, filed 1/14/76; Order 1, § 402-28-040, filed 1/8/69; Rules (part), filed 10/26/66.]
PDF246-225-060
Radiographic systems other than fluoroscopic, dental intraoral, or veterinary systems—Beam limitation.
The useful beam shall be limited to the area of clinical interest and show evidence of collimation. This shall be deemed to have been met if a positive beam limiting device has been properly used or if evidence of collimation is shown on at least three sides or three corners of the film, (for example, projections from the shutters of the collimator, cone cutting at the corners or a border at the film's edge).
(1) General purpose stationary and mobile X-ray systems.
(a) There shall be provided a means for stepless adjustment of the size of the X-ray field such that at least two dimensions of the X-ray field are independently variable. The minimum field size at a SID of 100 centimeters shall be equal to or less than ten by ten centimeters.
(b) Adequate means shall be provided for visually defining the perimeter of the X-ray field. The total misalignment of the edges of the visually defined field with the respective edges of the X-ray field along either the length or width of the visually defined field shall not exceed 2 percent of the distance from the source to the center of the visually defined field when the surface upon which it appears is perpendicular to the central axis of the X-ray beam.
(2) In addition to the requirements of WAC 246-225-060(1) above all stationary X-ray systems shall meet the following requirements:
(a) Means shall be provided to indicate when the axis of the X-ray beam is perpendicular to the plane of the image receptor and to align the center of the X-ray field with respect to the center of the image receptor to within 2 percent (5 percent for equipment manufactured prior to August 1974) of the SID. Dental lateral jaw examinations shall be excluded from this requirement;
(b) The beam-limiting device shall numerically indicate the field size in the plane of the image receptor to which it is adjusted;
(c) Indication of field size dimensions and SID's shall be specified in inches and/or centimeters;
(d) Indication of field size dimensions shall be such that aperture adjustments result in X-ray field dimensions in the plane of the image receptor to within 2 percent of the SID when the beam axis is perpendicular to the plane of the image receptor.
(3) Radiographic equipment designed for only one image receptor size at a fixed SID shall be provided with means to limit the field at the plane of the image receptor to dimensions no greater than those of the image receptor, and to align the center of the X-ray field with the center of the image receptor to within 2 percent of the SID.
(4) Special purpose X-ray systems.
(a) These systems shall be provided with means to limit the X-ray field in the plane of the image receptor so that such field does not exceed each dimension of the image receptor by more than 2 percent of the SID when the axis of the X-ray beam is perpendicular to the plane of the image receptor.
(b) These systems shall be provided with means to align the center of the X-ray field with the center of the image receptor to within 2 percent (5 percent for equipment manufactured prior to August 1974) of the SID.
(c) The above WAC 246-225-060 (4)(a) and 246-225-060 (4)(b) may be met with a system that meets the requirements for a general purpose X-ray system as specified in WAC 246-225-060(1) or, when alignment means are also provided, may be met with either:
(i) An assortment of removable, fixed-aperture, beam-limiting devices sufficient to meet the requirement for each combination of image receptor size and SID for which the unit is designed (each such device shall have clear and permanent markings to indicate the image receptor size and SID for which it is designed); or
(ii) A beam-limiting device having multiple fixed apertures sufficient to meet the requirement for each combination of image receptor size and SID for which the unit is designed. Permanent, clearly legible markings shall indicate the image receptor size and SID for which each aperture is designed and shall indicate which aperture is in position for use.
[Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-060, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-060, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 83-19-050 (Order 2026), § 402-28-051, filed 9/16/83. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-051, filed 12/8/80; Order 1084, § 402-28-051, filed 1/14/76. Formerly WAC 402-28-050 (part).]
PDF246-225-070
Radiographic systems other than fluoroscopic, dental intraoral, or veterinary systems—Radiation exposure control devices.
(1) Timers. Means shall be provided to terminate the exposure at a preset time interval, preset product of current and time, a preset number of pulses, or a preset radiation exposure to the image receptor. In addition, it shall be impossible to make an exposure when the timer is set to a zero or off position if either position is provided.
(2) X-ray control (exposure switch):
(a) A control which shall be the equivalent of a dead-man switch, shall be incorporated into each X-ray system such that an exposure can be terminated at any time except for:
(i) Exposure of one-half second or less, or
(ii) During serial radiography when means shall be provided to permit completion of any single exposure of the series in process.
(b) Each X-ray control shall be located in such a way as to meet the following requirements:
(i) Stationary X-ray systems shall be required to have the X-ray exposure switch permanently mounted in a protected area so that the operator has no choice but to remain in that protected area during the entire exposure;
(ii) Mobile and portable X-ray systems shall have:
(A) An exposure cord which can extend for a minimum of 12 feet from the patient; or
(B) A protective barrier of 0.25 millimeter lead equivalent between the patient and the operator.
(c) Each X-ray control shall provide visual evidence to the operator that X-rays are being produced and an audible signal that the exposure has terminated.
(3) Automatic exposure controls (phototimers). When an automatic exposure control is provided:
(a) Indication shall be made on the control panel when this mode of operation is selected;
(b) When the X-ray tube potential is equal to or greater than 50 kVp, the minimum exposure time for field emission equipment rated for pulsed operation shall be equal to or less than the interval equivalent to two pulses;
(c) The minimum exposure time for all equipment other than that specified in WAC 246-225-070 (3)(b) shall be equal to or less than 1/60 second or a time interval required to deliver 5 mAs, whichever is greater.
(4) Timer reproducibility. With a timer setting of 0.5 seconds or less, the difference between the maximum exposure time (Tmax) and the minimum exposure time (Tmin) shall be less than or equal to 10% of the average exposure time (T), when four timer tests are performed:
(Tmax - Tmin) ≤ 0.1T |
[Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-070, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-070, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 83-19-050 (Order 2026), § 402-28-052, filed 9/16/83. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-052, filed 12/8/80; Order 1084, § 402-28-052, filed 1/14/76. Formerly WAC 402-28-050 (part).]
PDF246-225-080
Radiographic systems other than fluoroscopic, dental intraoral, or veterinary systems—Source-to-skin or receptor distance.
(1) Limitation. All radiographic systems shall be provided with a durable, securely fastened means to limit the source-to-skin distance to not less than 23 centimeters. The requirement can be met when the collimator or cone provides the required limits.
(2) Source to receptor distance measuring device. All radiographic systems shall be provided with a device or reference, other than a collimator light localizer, which will indicate the selected source to image receptor distance (SID) to within 2 percent of the indicated SID.
[Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-080, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 83-19-050 (Order 2026), § 402-28-053, filed 9/16/83. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-053, filed 12/8/80; Order 1084, § 402-28-053, filed 1/14/76. Formerly WAC 402-28-050 (part).]
PDF246-225-090
Radiographic systems other than fluoroscopic and dental intraoral—Exposure reproducibility.
The exposure produced shall be reproducible to within the following criterion: When all technique factors are held constant, the coefficient of variation shall not exceed 0.05.
(1) For manual exposure control mode, this shall be deemed to have been met if when four exposures at identical technique factors are made, the difference between the maximum exposure value (Emax) and the minimum exposure value (Emin) shall be less than or equal to 10% of the average exposure (E):
(Emax) - (Emin) ≤ 0.10E |
(2) For phototimed exposure control mode, this shall be deemed to have been met if when four exposures at identical technique factors are made, the difference between the maximum exposure value (Emax) and the minimum exposure value (Emin) shall be less than or equal to 10% of the average exposure (E):
(Emax) - (Emin) ≤ 0.1E |
The four exposures are to be made under the following conditions in phototimed mode:
(a) The kV is held constant.
(b) The mA, if selectable, is held constant.
(c) The selected density, if selectable, is held constant.
(d) Selection of phototimer radiation detectors (single or multiple detectors selected), if available, is varied for each of the four exposures.
(e) The same attenuator is placed in the X-ray field between the selected phototimer radiation detectors (photocells) and the radiation detector used to determine the four exposure values.
(f) The selected phototimer radiation detectors (photocells) are within the X-ray field during each exposure measurement and are covered completely by the attenuator.
(3) Systems employing deliberately mismatched phototimed cells are permitted, providing written specifications for the mismatch are available for inspection.
[Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-090, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-090, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 83-19-050 (Order 2026), § 402-28-054, filed 9/16/83. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-054, filed 12/8/80; Order 1084, § 402-28-054, filed 1/14/76. Formerly WAC 402-28-050 (part).]
PDF246-225-100
Radiographic systems—Standby radiation from capacitor energy storage equipment.
Radiation emitted from the X-ray tube when the exposure switch or timer is not activated shall not exceed a rate of 2 milliroentgens per hour at 5 centimeters from any accessible surface of the diagnostic source assembly, with the beam-limiting device fully open.
PDF246-225-120
Therapeutic X-ray installations less than 1 MeV.
(1) Equipment requirements.
(a) Leakage radiation. When the tube is operated at its leakage technique factors, the leakage radiation shall not exceed the value specified at the distance specified for the classification of that X-ray system:
(i) Contact therapy systems. Leakage radiation shall not exceed 100 milliroentgens per hour at five centimeters from the surface of the tube housing assembly;
(ii) Zero to one hundred fifty kVp systems. Systems shall have a leakage radiation which does not exceed one roentgen in one hour at one meter from the source;
(iii) One hundred fifty-one to nine hundred ninety-nine kVp systems. The leakage radiation shall not exceed one roentgen in one hour at one meter from the source except systems that operate in excess of 500 kVp may have a leakage radiation at one meter from the source equivalent to the exposure within one hour of the useful beam at one meter from the source multiplied by a factor of 0.001.
(b) Permanent beam limiting devices. Permanent fixed diaphragms or cones used for limiting the useful beam shall provide the same or higher degree of protection as that required by the tube housing assembly.
(c) Removable and adjustable beam limiting devices.
(i) Removable beam limiting devices shall, for the portion of the useful beam to be blocked by these devices, transmit not more than one percent of the original X-ray beam at the maximum kilovoltage and maximum treatment filter;
(ii) Adjustable beam limiting devices installed after the effective date of this section shall meet the requirements of (c)(i) of this subsection;
(iii) Adjustable beam limiting devices installed before the effective date of this section shall, for the portion of the X-ray beam to be blocked by these devices, transmit not more than five percent of the original X-ray beam at the maximum kilovoltage and maximum treatment filter.
(d) Filter and wedge systems. Filter systems shall meet the following requirements:
(i) Filters cannot be accidently displaced from the useful beam at any possible tube orientation;
(ii) Each filter is marked as to its material of construction and its thickness or wedge angle for wedge filters;
(iii) It shall be possible for the operator to determine the presence or absence of each filter in the useful beam when the operator is at the control panel, either by display at the control panel or by direct observation; and
(iv) The filter insertion slot opening shall be covered with an attenuator equivalent to four-pound lead under operating conditions.
(e) Tube immobilization. The tube housing assembly shall be capable of being immobilized during stationary treatments.
(f) Focal spot marking. The tube housing assembly shall be so marked that it is possible to determine the location of the focal spot to within five millimeters, and such marking shall be readily accessible for use during calibration procedures.
(g) Timer.
(i) A timer shall be provided which has a display at the treatment control panel. The timer shall be graduated in minutes and fractions of minutes. The timer shall have a preset time selector and a means of determining elapsed time;
(ii) The timer shall be a cumulative timer which activates with radiation and retains its reading after irradiation is interrupted or terminated;
(iii) The timer shall terminate irradiation when a preselected time has elapsed;
(iv) The timer shall permit accurate presetting and determination of exposure times as short as 1 second;
(v) The timer shall terminate irradiation when set to zero;
(vi) The timer shall not activate until the shutter is opened, when patient irradiation is controlled by a shutter mechanism.
(h) Control panel functions. The control panel, in addition to the displays required in other provisions of this chapter, shall have:
(i) An indication of whether X-rays are being produced;
(ii) Means for indicating kV and X-ray tube current;
(iii) The means for terminating an exposure at any time;
(iv) A locking device which will prevent unauthorized use of the X-ray system; and
(v) For X-ray equipment manufactured after the effective date of this section, a positive display of specific filter(s) in the beam.
(i) Source-to-patient distance. There shall be means of determining the source-to-patient distance to within five millimeters.
(j) Shutters. Unless it is possible to bring the X-ray output to the prescribed exposure parameters within five seconds, the entire useful beam shall be automatically attenuated by a shutter having a lead equivalency not less than that of the tube housing assembly. In addition:
(i) After the unit is at operating parameters, the shutter shall be controlled electrically by the operator from the control panel;
(ii) An indication of shutter position shall appear at the control panel.
(k) Low filtration X-ray tubes. Each X-ray system equipped with a beryllium or other low-filtration window shall be clearly labeled as such upon the tube housing assembly and at the control panel;
(l) Alignment. When the therapy X-ray system is equipped with a light field indicating the X-ray field, the misalignment of one field edge to the other shall not exceed one percent of any source-to-treatment distance.
(2) Facility design requirements for systems capable of operating above 50 kVp.
In addition to shielding adequate to meet requirements of chapters 246-235 and 246-221 WAC and the shielding plan review provisions of WAC 246-225-030, the treatment room shall meet the following design requirements:
(a) Warning lights. Treatment rooms to which access is possible through more than one entrance shall be provided with warning lights, in a readily observable position near the outside of all access doors, which will indicate when the useful beam is "on." Or, as an alternative, entrances other than the main one shall be equipped with interior locks, activated for the period of exposure, and the main entrance shall be under control of the operator.
(b) Voice communication. Provision shall be made for two-way aural communication between the patient and the operator at the control panel; however, where excessive noise levels make aural communication impractical, other methods of communication shall be used.
(c) Viewing systems. Windows, mirrors, closed-circuit television, or an equivalent system shall be provided to permit continuous observation of the patient during irradiation and shall be so located that the operator can observe the patient from the control panel. When the primary viewing system is by electronic means (e.g., television), an alternate viewing system shall be available for use in the event of electronic failure or treatment must be discontinued until repair is made. If treatment is to be discontinued, this policy shall be included in the written safety procedures. A copy of the safety procedures shall be provided to the operator.
(d) Additional requirements. Treatment rooms which contain an X-ray system capable of operating above 150 kVp shall meet the following additional requirements:
(i) All necessary shielding, except for any beam interceptor, shall be provided by fixed barriers;
(ii) The control panel shall be outside the treatment room;
(iii) All doors of the treatment room shall be electronically connected to the control panel such that X-ray production cannot occur unless all doors are closed;
(iv) When the doors referred to in (d)(iii) of this subsection are opened while the X-ray tube is activated:
(A) X-ray production shall terminate within one second; or
(B) The radiation at a distance of one meter from the source shall be reduced to less than 100 milliroentgens per hour within one second.
(v) After the radiation output of the X-ray tube has been affected by the opening of any door referred to in (d)(iii) of this subsection, it shall be possible to restore the X-ray system to full operation only upon:
(A) Closing the door; and subsequently
(B) Reinitiating the exposure at the control panel.
(e) Calibrations.
(i) The calibration of an X-ray system shall be performed at intervals not to exceed one year and after any change or replacement of components which could cause a change in the radiation output.
(ii) The calibration of the radiation output of the X-ray system shall be performed by a qualified expert who is physically present at the facility during such calibration.
(iii) Calibration of the radiation output of an X-ray system shall be performed with a calibrated instrument. The calibration of such instrument shall be traceable to a national standard. The instrument shall have been calibrated within the preceding two years.
(iv) The calibrations made pursuant to (e)(i) of this subsection shall be such that the dose at a reference point in soft tissue can be calculated to within ± five percent.
(v) The calibration of the X-ray system shall include, but not be limited to, the following determinations:
(A) The exposure rates for each combination of field size, technique factors, filter, and treatment distance used;
(B) The degree of alignment between the radiation field and the field indicated by the localizing device if such device is present; and
(C) An evaluation of the uniformity of the radiation field symmetry for the field sizes used and any dependence upon tube housing assembly orientation.
(vi) Records of calibration performed pursuant to (e) of this subsection shall be maintained by the registrant for two years after completion of the calibration.
(vii) A copy of the most recent X-ray system calibration shall be available for use by the operator at the control panel.
(f) Operating procedures.
(i) When a patient must be held in position for radiation therapy, mechanical supporting or restraining devices shall be used;
(ii) The tube housing assembly shall not be held by an individual during exposures;
(iii) No individual other than the patient shall be in the treatment room unless such individual is protected by a barrier sufficient to meet the requirements of chapter 246-221 WAC. No individual other than the patient shall be in the treatment room during exposures when the kVp exceeds 150;
(iv) The X-ray system shall not be used in the administration of radiation therapy unless the requirements of (e) of this subsection have been met.
[Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-120, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-120, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 87-01-031 (Order 2450), § 402-28-091, filed 12/11/86; WSR 83-19-050 (Order 2026), § 402-28-091, filed 9/16/83. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-091, filed 12/8/80.]
PDF246-225-130
X-ray and electron therapy systems with energies of one MeV and above.
Chapter 246-229 WAC except WAC 246-229-100 (3) and (4) shall apply to medical facilities using therapy systems with energies 1 MeV and above.
(1) Definitions. In addition to the definitions provided in WAC 246-225-010, the following definitions shall be applicable to this section.
(a) "Applicator" means a structure which indicates the extent of the treatment field at a given distance from the nominal source and which may or may not incorporate an additional beam-limiting device.
(b) "Beam scattering foil" means a device which scatters and flattens a beam of electrons.
(c) "Central axis of the beam" means a line passing through the origin of the source and the center of the plane figure formed by the edge of the secondary collimating jaws when in a symmetric mode.
(d) "Dose monitoring system" means a system of devices for the detection and display of quantities of radiation.
(e) "Dose monitor unit" means a unit from which the absorbed dose can be calculated.
(f) "Existing equipment" means therapy systems subject to this section which were manufactured on or before the effective date of these regulations.
(g) "Field flattening device" means an absorber used to homogenize the dose rate over the area of a useful beam of X-rays.
(h) "Field size" means the dimensions of an area in a plane perpendicular to the specified direction of the beam of incident radiation at a maximum dose depth. Determine dimensions by fifty percent decrement lines.
(i) "Gantry" means that part of the system supporting and allowing possible movements of the radiation head.
(j) "Interruption of irradiation" means the stopping of irradiation with the possibility of continuing irradiation without resetting of the operating conditions at the control panel.
(k) "Isocenter" means a fixed point in space located at the intersection of the rotation axes of the principal movements of the therapy system.
(l) "Moving beam therapy" means radiation therapy with relative displacement of the useful beam and the patient during irradiation.
(m) "New equipment" means systems subject to this section which were manufactured after effective date of these regulations.
(n) "Nominal source" means a point from which radiation originates.
(o) "Normal treatment distance" means the distance between the virtual source and a reference point on the central axis of the beam. The reference is located at a position on the central axis at a specified distance from the nominal source.
(p) "Patient" means an individual subjected to examination and treatment.
(q) "Phantom" means a volume of material behaving in a manner similar to tissue with respect to the attenuation and scattering of radiation.
(r) "Primary dose monitoring system" means a system which will monitor the quantity of radiation produced during irradiation and which will terminate irradiation when a preselected number of dose monitor units have been acquired.
(s) "Radiation treatment prescription" means the absorbed dose which is intended to be delivered to the treatment volume.
(t) "Radiation head" means the structure from which the useful beam emerges.
(u) "Redundant dose monitoring combination" means a combination of two dose monitoring systems in which both systems are arranged to terminate irradiation in accordance with a preselected number of dose monitor units.
(v) "Secondary dose monitoring system" means a system which will terminate irradiation in the event of failure of the primary system.
(w) "Shadow tray" means a device attached to the radiation head to support auxiliary beam limiting material.
(x) "Stationary beam therapy" means radiation therapy without relative displacement of the useful beam and the patient during irradiation.
(y) "Target" means that part of a radiation source which intercepts a beam of accelerated particles with subsequent emission of other radiation.
(z) "Termination of irradiation" means the stopping of irradiation in a fashion which will not permit continuance of irradiation without the resetting of operating conditions at the control panel.
(aa) "Treatment field" means the cross-sectional area of the patient's tissue which is to be irradiated.
(bb) "Treatment volume" means that portion of the patient's body which is to be irradiated.
(2) Requirements for equipment.
(a) Leakage radiation to the patient area.
(i) New equipment shall meet the following requirements:
(A) For all operating conditions, the dose equivalent in rem due to leakage radiation, including X-ray and electrons, but excluding neutrons, at any point in a circular plane of two meters radius centered on and perpendicular to the central axis of the beam at the normal treatment distance and outside the maximum useful beam, shall not exceed 0.1 percent of the maximum dose equivalent in rem of the unattenuated useful beam measured at the point of intersection of the central axis of the beam and the plane surface. Measurements shall be averaged over an area up to but not exceeding one hundred square centimeters at the positions specified; and
(B) For each system the registrant shall determine, or obtain from the manufacturer, the leakage radiation existing at the positions specified in (a)(i)(A) of this subsection for specified operating conditions. Records for leakage radiation shall be maintained at the installation for inspection by the department.
(ii) Existing equipment (that installed prior to the effective date of the regulations) shall meet the following requirements:
(A) The leakage radiation, excluding neutrons, at any point in the area specified by (a)(i)(A) of this subsection, where such area intercepts the central axis of the beam one meter from the nominal source, shall not exceed 0.1 percent of the maximum dose equivalent in rems of the unattenuated useful beam measured at the point of intersection of the central axis of the beam and the surface of the reference circular plane. Measurements shall be averaged over an area up to but not exceeding one hundred square centimeters at the positions specified.
(B) For each system, the registrant shall determine, or obtain from the manufacturer, the leakage radiation existing at the positions specified in (a)(ii)(A) of this subsection for specified operating conditions. Records for radiation leakage shall be maintained at the installation for inspection by the department.
(b) Leakage radiation outside the patient area.
(i) The dose equivalent in rem due to leakage radiation, except in the area specified in (a) of this subsection, when measured at any point one meter from the path of the charged particle, before the charged particle strikes the target or window, shall not exceed 0.1 percent for X-ray leakage of the maximum dose equivalent in rems of the unattenuated useful beam measured at the point of intersection of the central axis of the beam and the circular plane specified in (a) of this subsection.
(ii) The registrant shall determine, or obtain from the manufacturer, the actual leakage radiation existing at the positions specified in (a) of this subsection for specified operating conditions. Measurements shall be averaged over an area up to but not exceeding one hundred square centimeters at the positions specified.
(c) Beam-limiting devices. Secondary beam-limiting devices shall be provided and such devices shall transmit no more than two percent of the useful beam for the portion of the useful beam attenuated by the beam-limiting device. The neutron component of the useful beam shall not be included in this requirement.
(d) Beam-modifying devices.
(i) When the absorbed dose rate information required by subsection (2)(q) of this section is dependent on operation with a beam-flattening or beam-scattering device in place, the device shall be removable from the machine only by the use of tools.
(ii) In systems using interchangable beam-flattening devices or beam-scattering foils:
(A) Irradiation shall not be possible until a selection of beam-modifying device is made and verified at the treatment control panel;
(B) An interlock system shall be provided to prevent irradiation when the beam-modifying device selected is not in the correct position; and
(C) A display at the control panel shall indicate what beam-modifying device is selected.
(e) Wedges.
(i) Presence of wedges in the beam shall be indicated at the control panel, by direct observation or by electronic means.
(ii) Each wedge removable from the system shall be clearly identified as to that wedge's material of construction, thickness, and wedge angle.
(iii) An interlock shall be provided to prevent irradiation when a wedge selection carried out in the treatment room does not agree with the wedge selection indicated at the control panel.
(f) Beam quality. The registrant shall obtain from the therapy X-ray system manufacturer, and have available, the following information:
(i) At various beam energies, the X-ray absorbed dose expressed as a fraction of maximum absorbed dose;
(ii) At various beam energies, the absorbed dose at the surface of the skin as a fraction of the maximum absorbed dose; and
(iii) The maximum percentage absorbed dose due to stray neutrons in the useful beam at specified operating conditions.
(g) Beam monitors. Therapy systems shall be provided with radiation detectors in the radiation head.
(i) New equipment shall be provided with two or more radiation detectors. The detectors shall be incorporated into two monitoring systems arranged either as a primary/primary combination or as a primary/secondary combination.
(ii) Existing equipment shall be provided with one or more radiation detectors. The detector shall be incorporated into a primary system.
(iii) The detectors and system where the detector is incorporated shall meet the following requirements:
(A) Each primary system shall have a detector which is a transmission full-beam detector placed on the patient side of beam-modifying devices;
(B) The detectors shall be removable only with tools and shall be interlocked to prevent incorrect positioning;
(C) Each detector shall be capable of independently monitoring and controlling the useful beam;
(D) Each detector shall form part of a dose-monitoring system from whose readings in dose monitor units the absorbed dose, at a reference point in the treatment volume can be calculated;
(E) For new equipment, the design of the dose-monitoring systems of subsection (2)(i) of this section shall assure the malfunctioning of one system shall not affect the correct functioning of the second system. In addition, the failure of an element common to both systems shall terminate irradiation.
(F) Each dose monitoring system shall have a legible display at the treatment control panel. Each display shall:
(I) Maintain a reading until intentionally reset to zero;
(II) Have only one scale and no scale multiplying factors in new equipment; and
(III) Utilize a design so increasing dose is displayed by increasing numbers and shall be designed so, in the event of an overdosage of radiation, the absorbed dose may be accurately determined under normal conditions of use or foreseeable failures.
(G) In the event of power failure, the dose-monitoring information required in subsection (2)(i) of this section displayed at the control panel at the time of failure shall be retrievable in one or more systems.
(h) Beam symmetry.
(i) A therapy machine installed after the effective date of these regulations shall have the capability of comparing the dose rates in each of the four quadrants of the central eighty percent of the useful beam.
(ii) Beam symmetry information shall be displayed at the treatment control panel making possible the following differential between quadrants:
(A) Five percent for straight-through accelerators; and
(B) Three percent for bending-magnet accelerators.
(iii) Beam asymmetry in excess of a ten percent quadrant differential shall cause treatment to terminate, or shall prevent irradiation.
(i) Selection and display of dose monitor units.
(i) Irradiation shall not be possible until a selection of a number of dose monitor units is made at the treatment control panel.
(ii) After useful beam termination, it shall be necessary manually to reset the preselected dose monitor units before treatment is reinitiated.
(iii) The preselected number of dose monitor units shall be displayed at the treatment control panel until reset manually for the next irradiation.
(j) Termination of irradiation by the dose monitoring system.
(i) Each of the required monitoring systems shall be capable of independently terminating an irradiation. Provision shall be made to test the correct operation of each system.
(ii) Each primary system shall terminate irradiation when the preselected number of dose monitor units is detected by the system.
(iii) Each secondary system shall terminate irradiation when a maximum of the preselected number of dose monitor units plus forty is detected by the system.
(iv) For new equipment, indicators on the control panel shall show which monitoring system terminated the beam.
(k) Interruption switches. It shall be possible to interrupt irradiation and equipment movements at any time from the operator's position at the treatment control panel. Following any interruption, it shall be possible to restart irradiation by operator action without any reselection of operating conditions. If any change is made of a preselected value during an interruption, the equipment shall go to termination condition.
(l) Termination switches. It shall be possible to terminate irradiation and equipment movements, or go from an interruption condition to termination conditions, at any time from the operator's position at the treatment control panel.
(m) Timer.
(i) A timer shall be provided which has a display at the treatment control panel. The timer shall be graduated in minutes and decimals of minutes. The timer shall have a preset time selector and an elapsed time indicator.
(ii) The timer shall be a cumulative timer which switches on and off with the radiation and retains its reading after irradiation is interrupted or terminated. It shall be necessary to zero and subsequently reset the elapsed time indicator and the preset time selector after irradiation is terminated before irradiation shall again be possible.
(iii) The timer shall terminate irradiation when a preselected time has elapsed if the dose monitoring systems fail to terminate irradiation.
(n) Selection of radiation type. Equipment capable of both X-ray therapy and electron therapy shall meet the following requirements:
(i) Irradiation shall not be possible until a selection of radiation type is made at the treatment control panel;
(ii) An interlock system shall be provided to insure that the equipment can emit only the selected radiation type;
(iii) An interlock system shall be provided to prevent irradiation if selected operations carried out in the treatment room do not agree with the selected operations carried out in the treatment control panel;
(iv) With the exception of a specified number of dose monitor units for the purpose of portal film exposures, an interlock system shall be provided to prevent irradiation with X-rays when electron applicators are in place and to prevent irradiation with electrons when accessories for X-ray therapy are in place; and
(v) The radiation type selected shall be displayed at the treatment control panel before and during irradiation.
(o) Selection of energy. Equipment capable of generating radiation beams of different energies shall meet the following requirements:
(i) Irradiation shall not be possible until a selection of energy is made at the treatment control panel;
(ii) An interlock system shall be provided to insure the equipment can emit only the energy of selected radiation;
(iii) An interlock system shall be provided to prevent irradiation if selected operations carried out in the treatment room do not agree with the selected operations carried out at the treatment control panel; and
(iv) The energy selected shall be displayed at the treatment control panel before and during irradiation.
(p) Selection of stationary beam therapy or moving beam therapy. Equipment capable of both stationary beam therapy and moving beam therapy shall meet the following requirements:
(i) Irradiation shall not be possible until a selection of stationary beam therapy or moving beam therapy is made at the treatment control panel;
(ii) An interlock system shall be provided to insure the equipment can operate only in the selected mode;
(iii) An interlock system shall be provided to prevent irradiation when any selected operations carried out in the treatment room do not agree with the selected operations carried out at the treatment control panel;
(iv) An interlock system shall be provided to terminate irradiation when the movement stops during moving beam therapy;
(v) Moving beam therapy shall be controlled so the required relationship between the number of dose monitor units and movement is obtained; and
(vi) The mode of operation shall be displayed at the treatment control panel.
(q) Absorbed dose rate. For new equipment, a system shall be provided from whose readings the absorbed dose rate at a reference point in the treatment volume can be calculated.3 In addition:
(i) The quotient of the number of dose monitor units by time shall be displayed at the treatment control panel; and
(ii) If the equipment can deliver, under any conditions, an absorbed dose rate at the normal treatment distance more than twice the maximum value specified by the manufacturer's anticipated dose rate for any machine parameters utilized, a device shall be provided which terminates irradiation when the absorbed dose rate exceeds a value twice the specified maximum. The value at which the irradiation is terminated shall be in a registrant-maintained record.
(r) Location of focal spot and beam orientation. The registrant shall determine, or obtain from the manufacturer, the location with reference to an accessible point on the radiation head of:
(i) The X-ray target or the virtual source of X-rays;
(ii) The electron window or the scattering foil;
(iii) All possible orientations of the useful beam.
(s) System interlock checks. Capabilities shall be provided to check radiation safety interlocks. When preselection of operating conditions requires action in the treatment room and at the treatment control panel, selection at one location shall not give a display at the other location until the requisite selected operations in both locations are completed.
(t) Facility and shielding requirements. In addition to chapter 246-221 WAC, the following design requirements shall apply:
(i) Except for entrance doors or beam interceptors, required barriers shall be fixed barriers;
(ii) The treatment control panel shall be located outside the treatment room;
(iii) Windows, mirrors, closed-circuit television, or other equivalent viewing systems shall be provided to permit continuous observation of the patient during irradiation and shall be located so the operator may observe the patient from the treatment control panel. When the viewing system is by electronic means, for example, by television, an alternate viewing system shall be provided for use in the event of the primary system failure, or, alternatively, treatments shall be discontinued until the viewing system is again functional;
(iv) Provision shall be made for two-way aural communication between the patient and the operator at the treatment control panel. However, where excessive noise levels make aural communications impractical, other methods of communication shall be used;
(v) Treatment rooms to which access is possible through two entrances or more shall be provided with warning lights and shall indicate when the useful beam is "on" in a readily observable position near the outside of all access doors; and
(vi) Interlocks shall be provided so entrance doors shall be closed before treatment is initiated or continued. When the radiation beam is interrupted by any door opening, it shall be possible to restore the machine to operation only by closing the door and reinitiating exposure by manual action at the control panel.
(u) Surveys, calibrations, spot checks and operating procedures.
(i) Survey.
(A) New facilities, and existing facilities not previously surveyed, shall have a survey made by, or under the direction of, a qualified expert. Such surveys shall also be done after a change in the facility or equipment causing a significant increase in radiation hazard.
(B) The registrant shall obtain a written report of the survey from the qualified expert and the registrant shall transmit a copy of the report to the department.
(C) The report shall indicate instances where the installation, in the opinion of the qualified expert, is in violation of applicable regulations and shall cite the section violated.
(ii) Calibrations.
(A) The calibration of systems subject to this section shall be performed before the system is first used for irradiation of patient and thereafter at time intervals which do not exceed twelve months and after any change which significantly alters the calibration, spatial distribution, or other characteristics of the therapy beam.
(B) The calibration shall be performed by a qualified expert.
(C) Calibration of the dose equivalent of the therapy beam shall be performed with a measurement instrument of which the calibration is traceable to national standards of exposure or absorbed dose and which shall have been calibrated within the preceding two years.
(D) Calibrations made under subsection (2)(u)(ii) of this section shall require the dose at a reference point in soft tissue be calculated within ± 5 percent.
(E) The calibration of the therapy beam shall include, but not be limited to, the following determinations:
(I) Verification that the equipment is operating in compliance with the design specifications concerning the light localizer, the side light and back-pointer alignment with the isocenter, when applicable, variation in the axis of rotation for the table, gantry and jaw system, and beam flatness and symmetry at specified depths;
(II) The output factors in terms of dose per monitor unit or dose per minute at a specific depth in a phantom for the range of field sizes used, for each effective energy, and for each treatment distance used for radiation therapy;
(III) The congruence between the radiation field and the field indicated by the localizing device; and
(IV) The uniformity of the radiation field and its dependency upon the direction of the useful beam.
(F) Records of the calibration performed under subsection (2)(u)(ii) of this section shall be maintained by the registrant for two years after completion of the calibration.
(G) A copy of the latest calibration performed under subsection (2)(u)(ii) of this section shall be available for operator use.
(iii) Spot checks. Spot checks shall be performed on the system subject to this section. Such spot checks shall meet the following requirements:
(A) A qualified expert shall develop, in writing, spot check procedures;
(B) The measurements taken during spot checks shall demonstrate the degree of consistency of the operating characteristics affecting the radiation output of the system or the radiation delivered to a patient during a therapy procedure;
(C) The spot check procedures shall specify the frequency of tests or measurements performed;
(D) For systems where beam quality can vary significantly, spot checks shall include quality checks;
(E) Where a system has built-in devices which provide a self-check of any parameter during irradiation, the spot check procedures shall require the parameter be independently verified at specific time intervals;
(F) Erratic spot checks or inconsistent spot checks of calibration data shall be promptly investigated and corrected before the system is used for patient irradiation;
(G) When a spot check indicates a significant change in the operating characteristics of a system, as specified in the qualified expert's spot check procedures, the system shall be recalibrated as required under subsection (2)(u)(ii) of this section;
(H) Records of spot check measurements performed under subsection (2)(u)(iii) of this section shall be maintained by the registrant for a period of one year or for twice as long as the spot check cycle, whichever is greater;
(I) Operating procedures.
(I) No individual other than the patient shall be in the treatment room during treatment of a patient.
(II) If a patient must be held in position during treatment, mechanical supporting or restraining devices shall be used.
(III) The system shall not be used in the administration of radiation therapy unless subsection (2)(u)(i), (ii), and (iii) of this section are met.
3 | The radiation detectors specified under subsection (2)(g) of this section may form part of this system. |
[Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-130, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-130, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 87-01-031 (Order 2450), § 402-28-101, filed 12/11/86. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-101, filed 12/8/80.]
PDF246-225-140
Veterinary medicine radiographic installations.
(1) Equipment.
(a) The protective tube housing shall be of diagnostic type.
See WAC 246-225-040(4).
(b) Diaphragms, cones, or a stepless adjustable collimator shall be used for collimating the useful beam to the area of clinical interest and shall provide the same degree of protection as is required of the housing. Cones or diaphragms, if used, shall be marked with their field size and the distance at which they are to be used.
(c) The half-value layer (HVL) of the useful beam shall not be less than as shown in the following table:
Measured Potential (kilovolts peak) | Half-value Layer (millimeters of aluminum equivalent) | |
70 and below | 1.5 | |
71 | 2.1 | |
80 | 2.3 | |
90 | 2.5 | |
100 | 2.7 | |
110 | 3.0 | |
120 | 3.2 | |
(d) A device shall be provided to terminate the exposure after a preset time or exposure. It must not be possible for the device to allow an exposure when preset at "zero" or "off."
(e) A dead-man type of exposure switch shall be provided, together with an electrical cord of sufficient length, so that the operator can stand out of the useful beam and at least two meters from the animal during all X-ray exposures.
(f) Reproducibility requirements as described under WAC 246-225-090.
(2) Structural shielding. All wall, ceiling, and floor areas shall be equivalent to or provided with applicable protective barriers as required in WAC 246-225-030(1).
(3) Operating procedures.
(a) In any application in which the operator is not located behind a protective barrier, clothing consisting of a protective apron having a lead-equivalent of not less than 0.25 millimeters shall be worn by the operator and any other individuals in the room during exposures.
(b) No individual other than the operator shall be in the X-ray room while exposures are being made unless such individual's assistance is required.
(c) When an animal or film must be held in position during radiography, mechanical supporting or restraining devices should be used. If the animal must be held by an individual, that individual shall be protected with appropriate shielding devices, such as protective gloves and apron, and that individual shall be so positioned that no part of that individual's body will be struck by the useful beam. The requirements of WAC 246-221-090, Personnel monitoring, and WAC 246-225-020 (2)(h)(iv) apply to such individuals.
[Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-140, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-140, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 83-19-050 (Order 2026), § 402-28-110, filed 9/16/83. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-110, filed 12/8/80; Order 1084, § 402-28-110, filed 1/14/76; Order 1, § 402-28-110, filed 1/8/69; Rules (part), filed 10/26/66.]
PDF246-225-150
X-ray film developing requirements.
Compliance with this section is required of healing arts registrants and is designed to ensure the patient and operator exposure is minimized, and to produce optimum image quality and diagnostic information.
(1) Manual processing of films:
(a) The following relationship between temperature of the developer and development time must be used (standard chemistry only):
thermometer readings (degrees) | minimum developing times (minutes) | ||
c | f | ||
27- | 80 | 2 | |
79 | 2 | ||
78 | 2 1/2 | ||
77 | 2 1/2 | ||
24- | 76 | 3 | |
75 | 3 | ||
74 | 3 1/2 | ||
73 | 3 1/2 | ||
22- | 72 | 4 | |
71 | 4 | ||
70 | 4 1/2 | ||
69 | 4 1/2 | ||
20- | 68 | 5 | |
67 | 5 1/2 | ||
66 | 5 1/2 | ||
65 | 6 | ||
18- | 64 | 6 1/2 | |
63 | 7 | ||
62 | 8 | ||
61 | 8 1/2 | ||
16- | 60 | 9 1/2 | |
(b) Processing of film. All films shall be processed to achieve adequate sensitometric performance. This criterion shall be adjudged met if:
(i) Film manufacturer's published recommendations for time and temperature are followed; or
(ii) Each film is developed in accordance with the time-temperature chart as required under subdivision (a) of this subsection.
(c) Devices shall be available giving:
(i) The actual temperature of the developer; and
(ii) An audible or visible signal indicating the termination of a preset time (in minutes).
(d) Chemical-film processing control.
(i) Chemicals shall be mixed in accordance with the chemical manufacturer's recommendations.
(ii) Developer replenisher shall be periodically added to the developer tank based on the recommendations of the chemical or film manufacturer. Solution may be removed from the tank to permit the addition of an adequate volume of replenisher.
(iii) All processing chemicals shall be completely replaced at least every two months.
(2) Automatic film processors shall be set up and maintained so radiographic density and contrast are optimal. This criterion shall be adjudged met if:
(a) Film manufacturer's published specifications for time and temperature are followed. In the absence of such specifications, the film shall be developed using the following chart:
minimal required developer temerature | processor developer immersion time* | ||
°C | °F | Seconds | |
35 | 95 | 20 | |
34.5 | 94 | 21 | |
34 | 93 | 22 | |
33.5 | 92 | 23 | |
33 | 91 | 24 | |
32 | 90 | 25 | |
31.5 | 89 | 26 | |
31 | 88 | 27 | |
30.5 | 87 | 28 | |
30 | 86 | 29 | |
29.5 | 85 | 30 | |
* | Immersion time only, no cross-over time included. |
The specified developer temperature and immersion time shall be posted in the dark room or on the automatic processor; and
(b) Replenishment of the developer chemistry is optimal:
(i) The processor shall deliver an adequate rate of developer replenishment; and
(ii) For facilities with a low X-ray workload, standby replenishment, flood replenishment, or periodically sending prefixed films through the processor may be necessary.
(c) Sensitometric tests of processor performance demonstrate the processor is achieving radiographic density and contrast equal to other processor models operating at equivalent developer immersion time and developer temperatures and using comparable chemistry.
(3) Darkrooms. Darkrooms shall be constructed so film being processed, handled, or stored will be exposed only to light passed through a safelight filter. The filter shall be of the type specified by the film manufacturer. Bulb wattage in the safelight shall be no greater than fifteen watts. The safelight shall be mounted at least 1.2 meters (four feet) above work areas.
(4) The department shall make X-ray film development and darkroom tests as necessary to determine compliance with this section.
[Statutory Authority: RCW 70.98.050. WSR 94-01-073, § 246-225-150, filed 12/9/93, effective 1/9/94. Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-150, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-150, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 83-19-050 (Order 2026), § 402-28-990, filed 9/16/83; Order 1084, Appendix C (codified as WAC 402-28-990), filed 1/14/76.]
PDF246-225-160
Mammography.
(1) The use of a special purpose X-ray machine designed and used solely for mammography is required. Exempted from this requirement shall be X-ray equipment using xerography for evaluation of breast implant integrity.
(2) All mammographic calibration, evaluation, service, and quality control actions shall be documented in writing and maintained at the facility for a three-year period. Records must be easily accessible to operators of these X-ray units.
(3) All tests requiring the use of a breast phantom shall employ a phantom similar to or identical to the one required by the American College of Radiology for its mammography accreditation program.
(4) Machine requirements:
(a) Mammography X-ray machines must be evaluated upon any major component change and on a yearly basis by a qualified medical physicist. Evaluation shall document (but is not limited to) half-value layer (HVL), kVP accuracy, reproducibility, timer accuracy, resolution achieved with film in use at the facility, focal spot size, mA linearity, light versus X-ray field alignment, and patient exposures (glandular tissue dose) following the measurement protocol in NCRP Report No. 85 (using a breast phantom). This requirement shall include initial acceptance testing upon the X-ray system's installation prior to human use.
(b) The half-value layer (HVL) for film/screen mammography shall be between the values of measured kVp/100 and measured kVp/100 + 0.1 millimeters aluminum. The half-value layer for xerography shall be at least 1.2 mm but no greater than 1.6 mm of aluminum as measured at 50 kVP. The HVL shall include the contribution to filtration made by the compression device.
(c) Exposure reproducibility: Manual techniques. See WAC 246-225-090.
(d) Exposure reproducibility: Photo-timed techniques. Mammographic systems in the AEC mode shall be able to maintain constant film density to within an optical density of ± 0.3 of the average optical density over the range of clinically used kVps, using BR-12 or other breast equivalent material phantom thicknesses of 2 centimeters to 6 centimeters. If the facility has established a technique chart that utilizes varying technical factors for different breast thicknesses, those adjustments in technique may be used when complying with this requirement.
(e) Radiographic timers. See WAC 246-225-070.
(f) kVP accuracy: The kVP accuracy published by the X-ray machine manufacturer shall be maintained at the specified level. For determination of actual versus indicated kVP, the manufacturer's recommendations for testing shall be followed.
(g) mA linearity. See WAC 246-225-040(10).
(h) All special purpose X-ray machines designed solely for mammography and installed after January 1, 1992, shall be equipped with a milli-ampere-second (mAs) read-out device, registering after each phototimed exposure. Alternatively, a means of determining mAs after each exposure shall be provided.
(i) Beam limitation:
(i) Mammographic systems shall be provided with means to limit the useful beam such that the X-ray field at the plane of the image receptor does not extend beyond any edge of the image receptor at any designed SID except the edge of the image receptor designed to be adjacent to the chest wall where the X-ray field may not extend beyond such edge by more than two percent of the SID.
(ii) Beam limiting devices consisting of an assortment of fixed, removable cones sufficient to meet the requirement for each combination of image receptor size and SID for which the unit is designed shall have clear and permanent markings to indicate the image receptor size and SID for which it is designed.
(iii) When the beam limiting device and image receptor support device are designed to be used to immobilize the breast during a mammographic procedure and the SID may vary, the SID indication specified in WAC 246-225-060 (4)(c)(i) and (ii) shall be the maximum SID for which the beam limiting device or aperture is designed.
(iv) In the absence of a visually defined X-ray field each image receptor support shall have clear and permanent markings to indicate the maximum image receptor size for which it is designed.
(j) The combination of source-to-image distance, magnification, and focal spot size shall result in a radiographic resolution of at least 12 line pairs per millimeter. This standard applies to the mammographic, single emulsion film being used at the facility.
(k) The X-ray machine shall be equipped with a means of immobilizing and compressing the breast with a force of at least twenty-five pounds but no greater than forty pounds.
(l) Dedicated mammographic X-ray units are exempted from the requirements of WAC 246-225-030 (5)(b)(i) provided that appropriate operator shielding is employed (as defined by NCRP Report 49).
(m) Transmission limit for image receptor supporting devices used for mammography. For X-ray systems manufactured after September 5, 1978, which are designed only for mammography, the transmission of the primary beam through any image receptor support provided with the system shall be limited such that the exposure 5 centimeters from any accessible surface beyond the plane of the image receptor supporting device does not exceed 25.8 nanocoulombs per kilogram (0.1 milliroentgen) for each activation of the tube. Exposure shall be measured with the system operated at the minimum SID for which it is designed. Compliance shall be determined at the maximum rated peak tube potential for the system and at the maximum rated product of tube current and exposure time (mAs) for that peak tube potential. Compliance shall be determined by measurements averaged over an area of 100 square centimeters with no linear dimension greater than 20 centimeters.
(n) Maximum glandular doses. Glandular tissue dose for a cranio-caudal view of a 4.5 cm compressed breast using dose calculation methods found in NCRP Report # 85 shall not exceed the following:
Screen-film:
No grid | = | 1.5 milliGray (100 millirads)/projection |
Grid | = | 2.5 milliGray (300 millirads)/projection |
Xerox | = | 4.0 milliGray (400 millirads)/projection |
(5) A quality control program shall be written and implemented for all mammographic facilities. This shall include (but shall not be limited to) tests performed, testing frequency, testing protocol, control limits for each test, corrective actions taken, and equipment maintenance/service. Program requirements include:
(a) Daily tests:
Film processor control charts using a sensitometric/densitometric based measurement system shall be required for each day the mammographic machine is in operation. Single emulsion mammographic film shall be used for this evaluation. The sensitometer shall be one with a 21-step optical attenuator.
Parameters in daily film processor tests shall include:
(i) Speed index (mid-density):
Control limits ± 0.15 optical density
(ii) Contrast index (density difference):
Control limits ± 0.15 optical density
(iii) Base + fog:
Maximum density shall not exceed 0.20 optical density.
(iv) Solution temperatures, using a digital thermometer that reads out in tenths of a degree and that is accurate to within ± 0.5°F.
Control limits ± 1.0 F
(b) Monthly tests:
(i) Chemical replenishment rates.
(ii) Image quality evaluation. The mammographic system shall be capable of providing an image of a 0.75 mm fiber, 0.32 mm speck group, and a 0.75 mm mass from an ACR, or equivalent, phantom on the standard mammographic image receptor system in use at the facility. Mammograms shall not be taken on patients if this minimum is not met. Any fibers, speck groups or masses larger than those specified shall also be imaged.
(c) Quarterly tests:
(i) Film/screen contact for all cassettes, using a 40-mesh copper screen.
(ii) Analyses of reject/repeat films.
(iii) Fixer retention in processed film.
(d) Semi-annual tests:
(i) Darkroom fog.
(ii) Compression device force.
(e) Yearly tests: See WAC 246-225-160 (4)(a).
(f) Cassette screens must be cleaned at least weekly.
(g) Records shall be maintained for quality control test equipment which requires calibration, and such calibrations shall be performed in accordance with recommendations of the manufacturer of the test equipment.
(h) Film processing. See WAC 246-225-150. A film processor that cannot be consistently made to operate within the control limits specified in (a) of this subsection shall not be used to process mammographic films.
(6) Operator competency:
(a) A mammographic machine operator shall be licensed, certified, or registered by the department as either:
(i) A health care practitioner, licensed under Title 18 RCW, if performing mammography is within the person's authorized scope of practice; or
(ii) A diagnostic radiologic technologist certified in accordance with chapter 18.84 RCW; or
(iii) An X-ray technician registered in accordance with chapter 18.84 RCW, with two or more years' experience in performing mammography and satisfactory completion of at least sixteen hours of training in mammographic positioning, mammographic quality assurance, and/or other related areas subject to approval by the department.
(b) A mammographic machine operator shall complete the equivalent of at least eight hours of training every twelve months covering such areas as mammographic positioning, mammographic quality assurance and other related areas subject to approval by the department.
(c) A mammographic machine operator shall meet the requirements of WAC 246-225-020 (2)(b) and 246-225-99920.
(7) Masking devices shall be made available to block extraneous light from the viewer's eye when the illuminated surface of the viewbox is larger than the exposed area on the film.
(8) Additional requirement for mobile mammography services:
The daily film processor performance testing required in subsection (5)(a) of this section shall apply to all film processors used by the mobile service. No processor shall be used unless it meets the control limits specified by subsection (5)(a)(i) through (iv) of this section.
[Statutory Authority: RCW 70.98.050. WSR 94-01-073, § 246-225-160, filed 12/9/93, effective 1/9/94; WSR 92-05-011 (Order 240), § 246-225-160, filed 2/7/92, effective 3/9/92.]
PDF246-225-99920
Appendix II—Determination of competency.
The following are areas in which the department considers it important that an individual have expertise for the competent operation of X-ray equipment.
(1) Familiarization with equipment.
(a) Identification of controls.
(b) Function of each control.
(c) The use of a technique chart.
(2) Radiation protection.
(a) Collimation.
(b) Filtration.
(c) Gonad shielding and other patient protection devices.
(d) Restriction of X-ray tube radiation to the image receptor.
(e) Personnel protection.
(f) Grids.
(3) Film processing.
(a) Film speed as relates to patient exposure.
(b) Film processing parameters.
(c) Quality assurance and quality control.
(4) Emergency procedures.
Termination of exposure in event of automatic timing device failure.
(5) Proper use of personnel dosimetry, if required.
(6) Understanding units of radiation.
[Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-99920, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-99920, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 83-19-050 (Order 2026), § 402-28-99003, filed 9/16/83; Order 1084, Appendix F (codified as WAC 402-28-99003), filed 1/14/76.]
PDF246-225-99930
Appendix III—Information to be submitted by persons proposing to conduct healing arts screening using ionizing radiation.
Persons requesting that the department approve a healing arts screening program shall submit the following information and evaluation:
(1) Name and address of the applicant and, where applicable, the names and addresses of agents within this state.
(2) Diseases or conditions and frequency for which the X-ray examinations are to be used.
(3) Description in detail of the X-ray examinations proposed in the screening program.
(4) Description of the population to be examined in the screening program, i.e., age, sex, physical condition, and other appropriate information.
(5) An evaluation of any known alternate methods not involving ionizing radiation which could achieve the goals of the screening program and why these methods are not used in preference to the X-ray examinations.
(6) An evaluation by a qualified expert of the X-ray system(s) to be used in the screening program. The evaluation by the qualified expert shall show that such system(s) satisfy all requirements of these regulations. The evaluation shall include a measurement of patient exposures from the X-ray examinations to be performed.
(7) A description of the diagnostic film quality control program.
(8) A copy of the technique chart for the X-ray examination procedures to be used.
(9) The qualifications of each individual who will be operating the X-ray system(s).
(10) The qualifications of the individual who will be supervising the operators of the X-ray system(s). The extent of supervision and the method of work performance evaluation shall be specified.
(11) The name and address of the individual who will interpret the radiograph(s).
(12) A description of the procedure to be used in advising the individuals screened and their private practitioners of the healing arts of the results of the screening procedure and any further medical needs indicated.
(13) A description of the procedures for the retention or disposition of the radiographs and other records pertaining to the X-ray examinations.
(14) An indication of the frequency of screening and the duration of the entire screening program.
[Statutory Authority: RCW 70.98.050 and 70.98.080. WSR 91-15-083 (Order 183), § 246-225-99930, filed 7/23/91, effective 8/23/91. Statutory Authority: RCW 43.70.040. WSR 91-02-049 (Order 121), recodified as § 246-225-99930, filed 12/27/90, effective 1/31/91. Statutory Authority: RCW 70.98.080. WSR 83-19-050 (Order 2026), § 402-28-99004, filed 9/16/83. Statutory Authority: RCW 70.98.050. WSR 81-01-011 (Order 1570), § 402-28-99004, filed 12/8/80.]